Calvary introduces robotic surgery
Local
The interaction of technology and orthopaedics was raised to the next level when Mako robot-guided surgeries were undertaken for the first time at the new Calvary Adelaide Hospital recently.
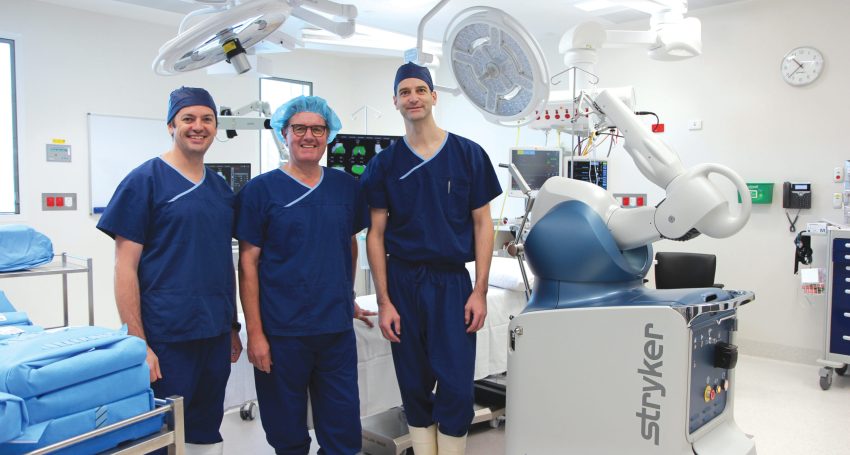
After the coronavirus restrictions on elective surgery were lifted in May, a team from the Wakefield Orthopaedic Clinic performed three surgeries at the Angas Street hospital using the Mako robot.
One of the members of the surgical team involved in the total knee, partial knee and hip replacements, was Mercedes College old scholar Dr Luke Mooney, who has trained extensively in the Mako technique.
He said the robot was a significant investment for Calvary in SA and it offered another option for patients at the hospital. Early research results show that using this method of surgery may result in patients having a shorter hospital stay and the need for less opiate medication for pain relief.
Advertisement
“Mako robotic assisted surgery is a method of joint replacement designed to increase the accuracy of implant positioning,” Dr Mooney told The Southern Cross.
“There are processes involved before and during surgery which are designed to improve the planning and execution of joint replacement surgery.
“For people undergoing the surgery we use a pre-operative CT scan which is used to plan the implant positioning. In hip surgery it allows planning for leg length and deformity correction which may be present for some patients, and in knees it allows accurate sizing of the implants.
“During the surgery, we attach tracking devices to the bones and carefully register the shape of the bones to ensure the robot understands where the bones are in space. We then perform the surgery using the information provided by the robot to insert the components.
“The robot is able to guide the cutting of bone and placement of implants to maximise accuracy and the patient outcome.”
While it is being used only for hip and knee replacements at this time, it is anticipated the technique will extend to shoulder replacements within the next year or so.
Advertisement
However, Dr Mooney stressed that robotic surgery wasn’t suitable in every instance and said surgeons at the Wakefield clinic had extensive experience in a range of methods of joint replacement surgery, including using conventional instruments, patient specific cutting jig technology, or computer navigation.
Attending Mercedes College from Year 5 to 12, Dr Mooney was determined to study medicine after he graduated in 2000.
“I have been very fortunate to be able to study medicine and orthopaedic surgery,” he said.
“I love my work and enjoy assisting patients to get back to doing the things they love by improving their joint pain and function. My career has enabled me to study and work interstate in Perth and overseas in Ireland and Canada, and it has introduced me to many inspiring people.”
Dr Mooney said his Catholic schooling had provided a great foundation for his life and career.
“The college uses the Mercy Keys – loyalty, integrity, compassion, justice, mutual respect and responsibility – to provide a strong value-centred education, reflecting the ethos of the Sisters of Mercy.
“I believe my time at Mercedes has helped me provide my patients with compassionate care,” he said.
A Mercedes Old Scholars’ Association council member in the first three years after graduating from school, Dr Mooney said he was looking forward to his 20-year graduation anniversary celebration this year and catching up with old friends.
Joining Dr Mooney in the history-making robot guided surgeries team was surgeon Dr Sam Benveniste and Dr Richard Clarnette from Wakefield Orthopaedic Clinic, anaesthetist Dr Indy Lin, scrub nurse Ashlee Schulze, anaesthetic nurse Nicole Benesh, scout nurse Erin Ronis and Stryker company representatives Heath Commane and Jake Sadauskas.












Comments
Show comments Hide comments